ADASRI collaborates with NIST to create artificial blood vessels to study effects of fluid flow on tissue
Research could be used to examine how experimental gum disease drugs affect vessel elasticity
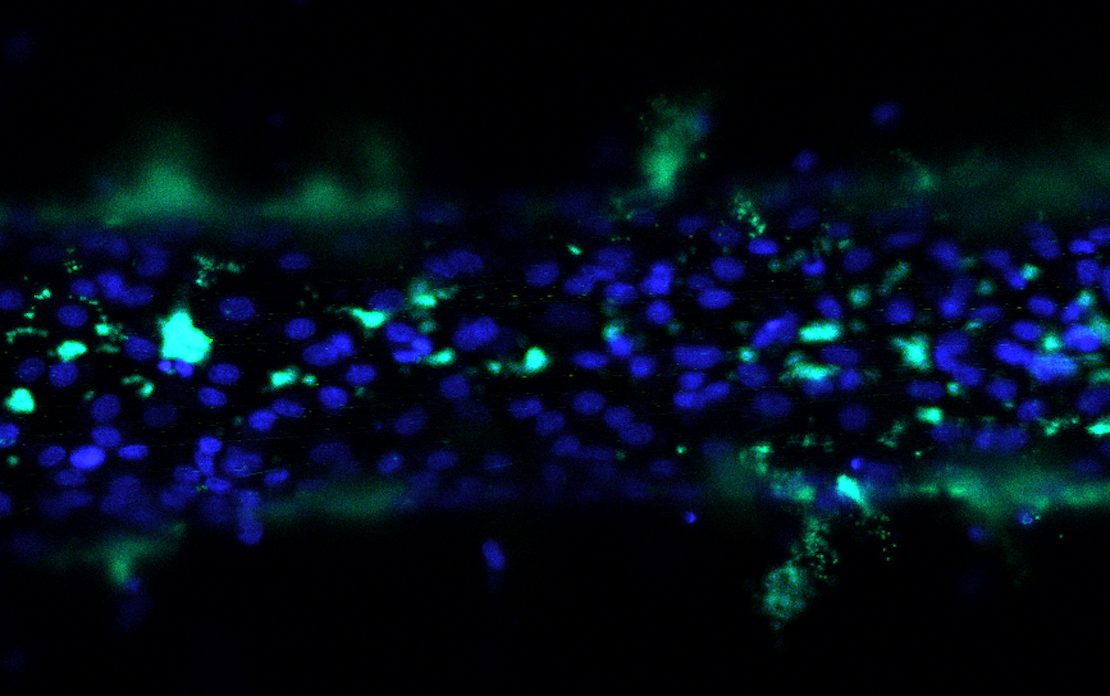
Researchers from the American Dental Association Science & Research Institute and National Institute of Standards and Technology collaborated to study how fluid flow affects the mechanical properties of biological tissue, including its elasticity and permeability.
The scientists 3D-printed small devices called microfluidic chambers that contained channels through which tiny quantities of fluid could flow and then passed human endothelial cells through the tube-shaped channels. The cells adhered to the walls of the channels, forming artificial blood vessels about the size of a large capillary with sides as thick as a single endothelial cell.
The researchers then pushed fluid through the channels and used fluorescent dye to track the resulting flow, capturing the process with a 3D confocal microscope. Their study showed the fluid particles could leak through the cell layer or get trapped in small pores.
This research could be helpful in understanding the effects of drugs on blood vessels, as well as how tissue resists inflammation, how capillaries regulate blood pressure and how tissue acts as a protective physical barrier.
"In the future, we could use these microfluidic chambers to study the way experimental drugs for treating gum disease affect the elasticity of blood vessels," said Stella (Styliani) Alimperti, Ph.D., a project leader with the ADASRI who worked with NIST on this study.
"Blood Vessel-on-a-Chip Examines the Biomechanics of Microvasculature" was published in November 2021 by the journal Soft Matter.



